
Joint Reconstruction, Part 1 – Expertise for Endoprosthetics
, roslerusa - Volver a la vista general
With more than $18 billion in annual worldwide sales, implants for joint reconstruction make up nearly 40 percent of all orthopedic product sales. More active lifestyles and increased life expectation continue to contribute to the rapid growth of this market segment.
Thanks to significant advancements on the material side and enhanced surface finishing technologies, artificial hips and knees can last more than 20 years before they must be replaced. Rosler Metal Finishing’s shot blasting and mass finishing capabilities are examples of processes and equipment that have and continue to evolve to accommodate the demand for increased endoprosthetics which are also known as orthopedic joint reconstruction implants.
These techniques play a key role in intermediate processing steps including cleaning, deburring/edge radiusing, surface smoothing, and surface preparation for coatings after casting, forging, machining, CNC grinding as well as placing the final finish on the implants before they are inserted.
Implant Basics
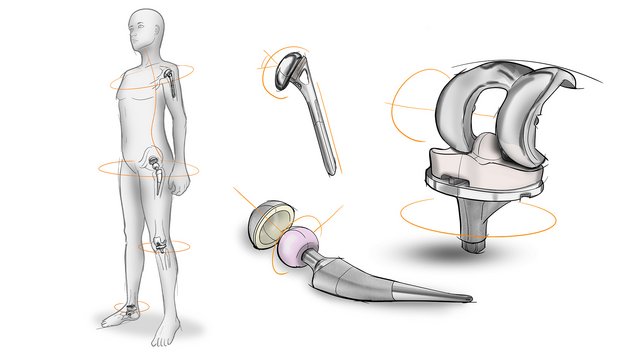
Quality standards for orthopedic implants are probably the most demanding of any industry, but, because joint reconstruction implants consist of two moving components interacting with each other, the requirements for these specific implants are even more rigorous.
Besides the right material choice and absolutely minimal dimensional tolerances, joint reconstruction implants must have a perfect surface finish. This often involves achieving two distinct finishes on a single component.
In the case of an artificial knee, the end of the femoral piece must be extremely smooth, as it must move freely on the tibia plate. Whereas the backsides of femoral and tibia plate need a textured, somewhat rougher surface to allow for osseointegration, the attachment of tissue and bone to the implant.
Prevalence & Longevity

As suggested by the name, the purpose of orthopedic joint reconstruction implants is to repair a damaged or replace a missing joint by inserting a manufactured medical device into the body.
Joint reconstruction is particularly challenging because the implants must allow free movement of the joint and, at the same time, must be firmly attached to the respective bones.
Accounting for nearly 90 percent of joint replacements, knee and hip replacements are by far the most common joint reconstruction procedures. Thanks to various technological breakthroughs, so-called “extremity” implants for jaws, shoulders, elbows, hands, and feet are increasingly performed as well.
Contrary to trauma implants, which may be removed after a bone has healed, the goal for joint reconstruction implants is to remain permanently in the body, at least as long as they provide a normal, pain-free function of the respective joint. The longevity of these implants has improved continually, and most joint replacements now have a life expectancy of more than 20 years.
Required Characteristics

Joint reconstruction implants are subject to the same zero-defect performance and reliability standards as any other implants, but, because two components are always interacting with each other, dimensional accuracy is of particular importance.
The finish of joint reconstruction implants must meet a variety of characteristics including:
- Biocompatibility – The implants must not be toxic, injurious, or physiologically reactive while avoiding immunological rejection. They must also resist corrosion in reaction to bodily fluids.
- High tensile strength and long-life span – Some joint implants such as knees and hips are exposed to considerable loads. They must withstand these loads for a lifetime without breaking.
- Low friction at the joint areas – Very smooth, polished surfaces are required on joint areas to promote range of motion.
- Rounded edges – Removing sharp edges from these implants help reduce the risk of ruptured blood vessels and blood clots during insertion as well as the healing process.
- High osseointegration – Implants attached to the bone must encourage the attachment of the surrounding bone tissue to the implant itself. This requires a somewhat textured, rougher surface.
- Low dimensional tolerances – The two implant components must meet and function precisely to ensure that the joint’s operation is not too tight or too loose.




